Important updates on the Sarawak VTE scoring system
O&G@SGH_Guidelines:01/2017
REVISED 2017 SARAWAK OBSTETRIC VTE RISK ASSESSMENT PROGRAM
A. Introduction
The Sarawak VTE Risk Assessment program was first introduced in all government hospitals in Sarawak from March 2013. In early 2014, it was also successfully implemented in most health clinics in the state.
The impact of this program was significant in terms of reducing maternal deaths due to pulmonary embolism (PE) in the state. In the 5 year period between 2008 till 2012, there were 15 maternal deaths attributed to PE. This was an average of 3 deaths per year. Since the implementation of program, the number of deaths attributed to PE has decreased to an average of 1 death per year. The program has also contributed to the reduction in the state’s maternal mortality ratio (MMR) to 9.3 per 100,000 live births in 2013, 16 per 100,000 in 2014 and 2015 respectively. This compares well to the national MMR which was estimated at 26 per 100,000 live births for the corresponding years.
The Green Top guideline 37a on ‘Reducing the risk of venous thromboembolism during pregnancy and the puerperium’ was published in April, 2015 by the Royal College of Obstetricians & Gynaecologists (RCOG), UK. It provided new clinical evidence that recommends a longer duration of VTE prophylaxis as well as new risk factors. The 2015 Sarawak Obstetric VTE Risk Assessment program incorporated these changes.
The changes meant that even higher percentage of women needed VTE prophylaxis. It is estimated about 4-6% of antenatal women and 40-45% of postnatal women were given VTE prophylaxis. However, this increase has not had the desired impact of further reducing incidences of maternal deaths attributed to VTE in the state. There is no registry for Obstetric VTE events in the state, thus the lack of data to assess the impact of the changes made in the 2015 Green Top Guidelines 37a.
The maternal deaths attributed to VTE in the state since the implementation of the program in 2013 are due to high risk women who should be given VTE prophylaxis but was not because of the failure to do a risk scoring.
The cost of the Obstetric VTE Risk Assessment program in the state was significantly higher following the 2015 revision. A relook at the program is necessary to ensure that it remains financially viable and to reduce the exceedingly high percentage of antenatal or postnatal women that needed to be on VTE prophylaxis.
There are existing Obstetric VTE risk assessment guidelines available in other developed nations which recommended different risk scoring systems. In Canada and the USA recommends only women at very high risk of VTE should be given prophylaxis.
The 2017 Sarawak Obstetric VTE Risk Assessment program would reflect a more practical approach with only higher risk women being recommended for VTE prophylaxis. The national 2 committee assigned to revise the Obstetric VTE guidelines had agreed to exclude most of VTE risk factors listed in the 2015 Green Top Guidelines 37a with an odds ratio (OD) of less than 3 (table 1).
The 5 main focus of having an effective program should be;
1 Ensuring that universal screening or risk scoring must be carried out accordingly
2 Ensuring all antenatal and postnatal women would be appropriately counselled on the higher risk of VTE during pregnancy and in the puerperium period. This must include the risk factors, signs & symptoms of VTE and prevention. It should be realized that the best screening program would only be able to identify 70% of those who may develop VTE.
3 Women at high risk of VTE should be given VTE prophylaxis
4 Those perceived at risk but not high enough to require VTE prophylaxis should be advised to use mechanical methods (e.g. anti-embolic stockings)
5 Training
B. REVISED 2017 OBSTETRIC VTE GUIDELINES
- The 2017 Sarawak Obstetric VTE Risk Assessment form (attachment 1)
| No. | VTE risk factor | Odds Ratio (OR) |
|---|---|---|
| 1 | Age > 35 | 1.3 |
| 2 | Parity > 3 | 2.4 |
| 3 | Smoking < 10/day | 2.1 |
| 4 | Preterm delivery < 37 weeks | 1.7 |
| 5 | Twins | 2.6 |
| 6 | Varicose veins | 2.4 |
Table 2: The 2017 Sarawak Obstetric VTE Risk Assessment recommendations for specific antenatal & postnatal VTE risk scores:
| Period | Score | Duration of thromboprophylaxis |
|---|---|---|
| Antenatal | > 4 | Consider giving from 1st trimester up to 6 weeks postnatal (give up to 6 weeks postnatal if there is a single risk with a score of 4. If a combination score of > 4, then give in antenatal period and up to 3 weeks postnatal then should be reviewed by a doctor if a further 3 weeks of prophylaxis is needed) |
| Antenatal | 3 | Consider prophylaxis from 28 weeks till 3 weeks postnatal |
| Postnatal | 2 | Consider prophylaxis for 10 days |
| Postnatal | > 2 | Consider prophylaxis for 10 days then review by a doctor if a further 11 days of prophylaxis is required (max 3 weeks) |
- Antenatal mothers requiring VTE prophylaxis should be coded yellow to ensure they are reviewed at least once by a FMS or an O&G specialist
- Postnatal mothers requiring VT prophylaxis should be coded green, to ensure they are reviewed at least once by a medical officer
- The recommended duration of VTE prophylaxis is different from the 2015 Sarawak Obstetric VTE Risk Assessment guidelines
- Mothers with a single score of 4 as listed in table 3, are considered as very high risk and should be considered for VTE prophylaxis from the 1st trimester up to 6 weeks postnatal
- Mothers with antenatal cumulative risk score of > 4 (in the absence of a very high risk factor) should be considered for VTE prophylaxis from the 1st trimester up to 3 weeks postnatal. They should then be reviewed by a medical officer to decide if an additional 3 weeks of prophylaxis is recommended. The use of anti-embolic stockings instead of the additional 3 weeks of VTE prophylaxis is an option, on the risk factors involved and patient’s wishes. Medical officers who are uncertain could consult a FMS or an O&G specialist.
- Mothers with a postnatal score of 2 should be considered for 10 days of VTE prophylaxis
- Mothers with a postnatal score > 2 should be considered 10 days of VTE prophylaxis but should be reviewed by a medical officer to decide if a further 11 days of VTE prophylaxis is recommended. The use of anti-embolic stockings instead of an additional 11 days of VTE prophylaxis is an option, based on the risk factors involved and the patient’s wishes. Medical officers who are uncertain should consult a FMS or an O&G specialist.
- A small stock of LMWH (e.g. clexane 40mg) should be made available in health clinics with FMS and in district hospitals without O&G specialists. This is to facilitate initiating VTE prophylaxis by medical officers or by FMS for antenatal or postnatal mothers that require VTE prophylaxis.
- LMWH are listed as A* category drug, thus while medical officers and FMS could prescribe and initiate VTE prophylaxis, it should mailed to an O&G specialist in the nearest hospital to be countersigned. Prior consultation with the O&G specialist is not necessary.
Table 3: List of ‘High Risk’ factors
| No | High Risk factors | Score |
|---|---|---|
| 1 | Previous VTE (estrogen related, recurrent, unprovoked) –Very High Risk | 4 |
| 2 | Previous VTE (provoked by major surgery or major accident) | 3 |
| 3 | Thrombophilia (anti thrombin deficiency) | 3 |
| 4 | Medical comorbidities (active SLE, severe heart disease, heart failure, nephrotic syndrome. Type 1 DM with nephropathy, inflammatory polyarthropathy, inflammatory bowel disease, cancer) | 3 |
| 5 | Current IVDU | 3 |
Table 4: List of transient ‘High Risk’ factors
| No | Transient high risk factors | Score |
|---|---|---|
| 1 | Ovarian hyperstimulation syndrome (OHSS) requiring admission | 4* |
| 2 | Hyperemesis gravidarum requiring admission | 4* |
| 3 | Surgery in pregnancy or puerperium (excluding ERPOC or T&S) | 4** |
- Antenatal mothers with transient transient high risk factors listed in table 4, require VTE prophylaxis.
- Those admitted and diagnosed with OHSS or hyperemesis gravidarum should be considered for VTE prophylaxis for the duration of their admission. Longer duration of prophylaxis is up to the attending clinician to decide.
- Those who had surgery beside ERPOC or toilet & suture in the antenatal and puerperium should be considered for VTE prophylaxis during their admission and up to an additional 10 days post-discharge.
- Transient factors are relevant only during that episode and should not add to the longer term overall risk score
C. WHICH ANTICOAGULANT AGENTS SHOULD BE USED FOR THROMBOPROPHYLAXIS?
- Low molecular weight heparins (LMWH) such as Tinzaparin (Innohep) & Enoxaparin (Clexane) are preferred
- Monitoring of platelet levels or anti-Xa levels is not necessary if LMWH is used as thromboprophylaxis unless her weight is less than 50Kg or more than 90Kg.
- LMWH is safe in breastfeeding
- Tinzaparin has a better renal safety profile compared to clexane
- Patients should be taught to self-administer LMWH
- Unfractionated heparin should ideally be administered by trained health personnel twice daily
- Long term unfractionated heparin use is associated with a very small increase risk of osteoporosis. It is also associated with heparin induced thrombocytopaenia and thrombosis.
- Patients on unfractionated heparin should have their platelet level checked at least once between day 5-8, if they are on a 10 -14 day prophylaxis. If they are on longer duration of prophylaxis, subsequent fortnightly FBC is recommended. If platelet level falls below 150K or reduce by 50%, then refer to a FMS or an O&G specialist.
- Fondaparinux should be reserved for women intolerant of heparin compounds. The efficacy and safety profile in pregnancy and breastfeeding mothers are yet to be determined. It has a longer half-life and no known antidote, so usage in the antenatal period carries risks.
- Low dose aspirin is not recommended for thromboprophylaxis in obstetric patients
- Warfarin use in pregnancy is restricted to a few situations where heparin is considered unsuitable, e.g. women with mechanical valve. While it is safe in breastfeeding, it is associated with several significant complications. The use must be under the supervision of an O&G specialist / Cardiologist / Haematologist.
- Dextran should be avoided in pregnancy because of the risk of anaphylactic reaction
D. PATIENTS WHO REFUSED VTE PROPHYLAXIS
- Counseling play an important role (consider further counseling by FMS or O&G specialist)
- Doctors in health centers without specialists – consult an O&G specialist or buddy specialist
- Upon failure to convince the patient;
- Use appropriate Anti-embolic stockings
- Advise on ambulation, avoidance of dehydration & to seek early treatment if feeling unwell
- Teach patients to identify signs & symptoms of DVT & PE
- Ensure ‘home visits’ by community midwife/nurse (use the attached nurse’s ‘checklist’ during home visits)
E. WHAT TO LOOK FOR DURING POSTNATAL HOME VISITS?
- Public health nurses should use the ‘checklist’ form during every postnatal home visits if the patient is on thromboprophylaxis (attachment 2)
- They should also check if the patient has been compliant with her injections (check the balance of injections).
- The mothers should be referred to the nearest clinic or hospital urgently if she has or display any of the signs and symptoms of DVT or PE. The nurse should try to assist in the arrangement to transfer the patient when the situation requires it.
- The mothers should be referred to see a doctor in the nearest clinic or admitted to the nearest hospital if she is unwell
- 2/3 of all pulmonary embolisms occur in the postnatal period. PE could still occur even if the patient is on VTE prophylaxis. The role of health doctors and nurses in being able to look for and identify the signs and symptoms of DVT/PE is an important one.
F. WHAT TO DO IF YOU SUSPECT YOUR PATIENT HAS DVT OR PE?
- Suspected DVT needs urgent attention & referral
- Suspected PE is a medical emergency!
- If suspected during ‘home visits’ – arrange to transfer the patient to the nearest specialist hospital. If this is via a clinic or a district hospital then refer to the guide below
- Suspected DVT/PE in health clinics/district hospital;
- Refer case to a specialist by phone
- Discuss about;
a. Heparinisation / anti-coagulation before transfer
b. Intubation (for suspected PE) before transfer
c. MO escort
- All suspected cases of DVT / PE should have treatment commenced upon clinical suspicion.
- Objective confirmation of DVT can wait until the equipment and its expertise becomes available.
- Diagnosis should not delay commencement of treatment (where available, 1st dose of anticoagulation therapy should be given prior to transfer)
- PE should be managed by a multi-disciplinary team in a specialist hospital
G. IMPORTANCE OF UNIVERSAL COUNSELING ON VTE IN PREGNANCY
- Only 70% of mothers whose death is attributed to VTE have significant risk factors.
- The 2017 Obstetric VTE Risk assessment form is geared towards recommending giving VTE prophylaxis to those at higher risk compared to the previous guidelines
- These points highlights the importance of appropriately counselling all pregnant women during their antenatal booking or VTE risk assessment on;
a. About VTE
b. Pregnancy and the puerperium increases the risk of VTE significantly
c. The role of VTE risk assessment and thromboprophylaxis
d. Signs & symptoms of DVT & PE
e. General advise on reducing risk of VTE
f. Provide VTE in pregnancy patient information leaflets
H. UPDATING & TRAINING OF HEALTHCARE PROVIDERS
- The healthcare providers (doctors and nursing staff) in government healthcare facilities in the state of Sarawak are generally well versed with the Obstetric VTE risk assessment program.
- The new 2017 Obstetric VTE program has to be distributed to all relevant health clinics and hospitals in the state and all relevant staff have to be briefed
- It is imperative that new doctors and nurses to any health facility are briefed on the program
This revised guideline should be implemented by January 2017 in all government health facilities in the State of Sarawak
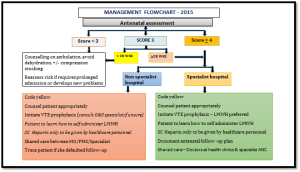
I. SARAWAK ‘VTE RISK ASSESSMENT IN PREGNANCY’ MANAGEMENT FLOW CHARTS:
1. Flowchart 1: Antenatal VTE assessment
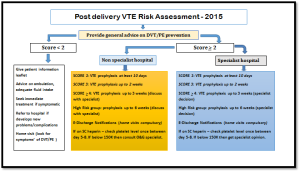
2. Flowchart 2: Post delivery VTE Risk assessment
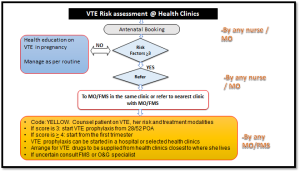
3. Flowchart 3: VTE Risk Assessment in health clinics
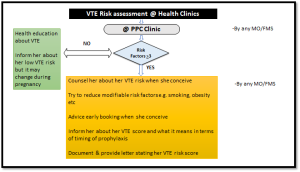
4. Flowchart 4: VTE Risk Assessment in PPC clinic
HOME VISITS THROMBOEMBOLISM CHECK LIST FOR ANTENATAL OR POSTNATAL July 2015